| Important questions for UPSC Pre/ Mains/ Interview:
1. What are India’s long-standing commitments on public health financing? 2. How does India compare globally in public health spending? 3. What trends emerged during and after the COVID-19 pandemic? 4. Why is declining Union government health spending a concern? 5. How are States driving health expenditure growth? 6. Has the Health and Education Cess strengthened health budgets? 7. What is the significance of cuts in Centrally Sponsored Health Schemes? 8. What are the implications for public health outcomes? 9. What are the key challenges in India’s health financing model? 10.What should be the way forward to strengthen health financing? |
Context
Recent data reveal that while States have increased health expenditure, the Union government’s health spending as a share of GDP has declined post-pandemic, raising concerns about fiscal priority to health.
Q1. What are India’s long-standing commitments on public health financing?
- India’s health financing framework recognises public spending as central to health outcomes.
- The National Health Policy 2017 committed to raising public health expenditure from 15% to 2.5% of GDP by 2025.
- A key design feature was a higher Union government share (around 40%) to support States.
- As of 2025–26, these targets remain unmet, signalling a gap between policy intent and budgetary prioritisation.
Q2. How does India compare globally in public health spending?
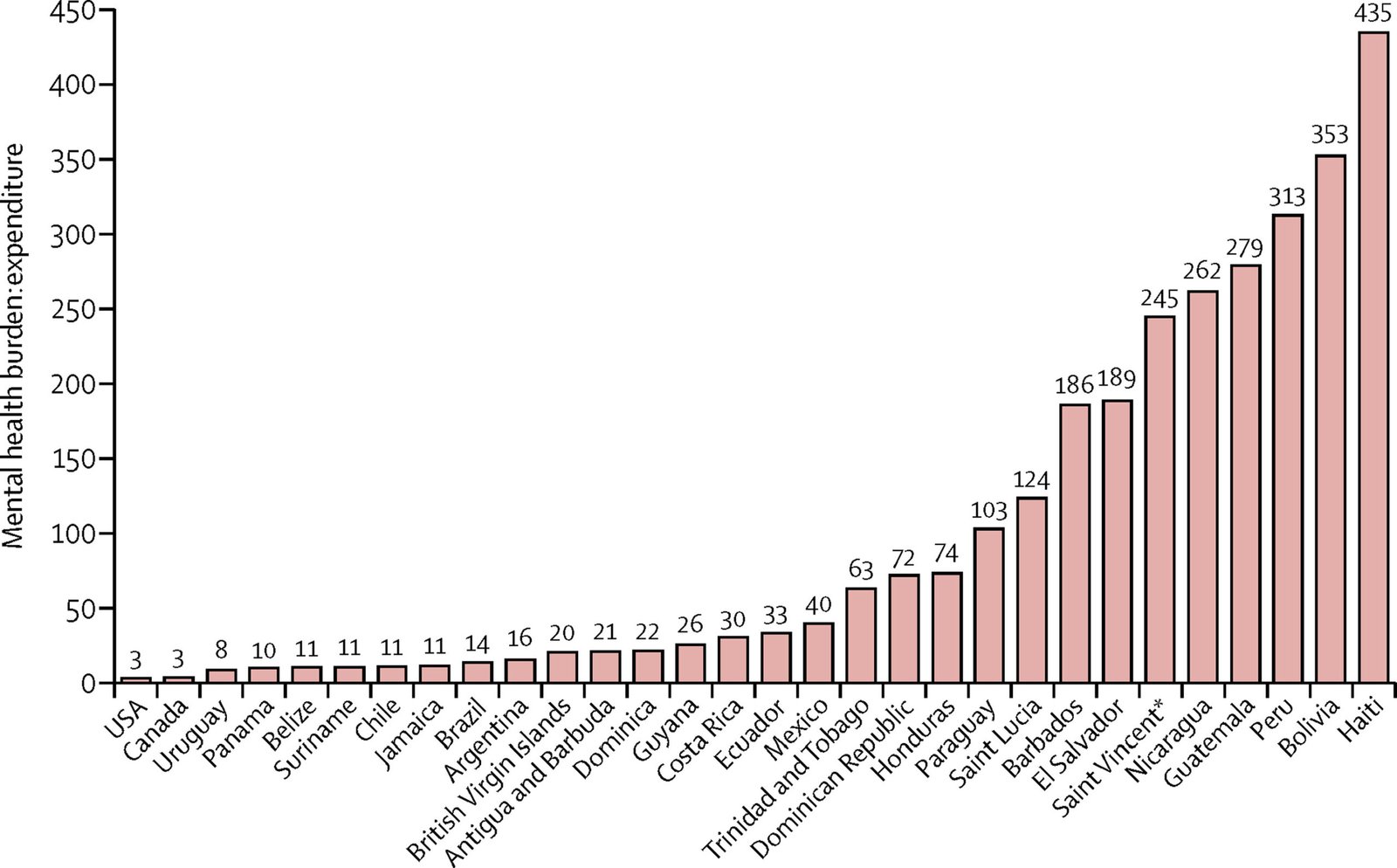
- India’s public health expenditure remains among the lowest in the world.
- Countries such as Bhutan, Sri Lanka, Thailand, and Malaysia spend significantly more per capita on public healthcare.
- Even among BRICS nations, India’s per capita public health spending is markedly lower.
- This structural underinvestment limits access, quality, and financial protection.
Q3. What trends emerged during and after the COVID-19 pandemic?
- During the pandemic, health spending as a share of GDP rose temporarily.
- However, this increase was largely driven by State governments, not sustained Union expansion.
- Post-pandemic, health expenditure growth has slowed, indicating that emergency prioritisation was not institutionalised.
Q4. Why is declining Union government health spending a concern?
- According to Reserve Bank of India data:
- Union health expenditure fell from 37% of GDP (2020–21) to 0.29% (2025–26 BE).
- In real terms, the 2025–26 allocation is 7% lower than actual spending in 2020–21.
- Health’s share in the Union Budget declined from 26% to 2.05%, reflecting relative de-prioritisation.
- This weakens the Centre’s ability to support nationwide health system strengthening.
Q5. How are States driving health expenditure growth?
- States and Union Territories have consistently increased health spending since 2017–18.
- State health expenditure rose from 67% of GDP to 1.1% by 2025–26.
- Health’s share in State budgets increased from 5% to 5.6%.
- However, since health is largely a State subject, States depend heavily on Union transfers—making reduced Central spending a structural constraint.
Q6. Has the Health and Education Cess strengthened health budgets?
- The Health and Education Cess (HEC) was introduced in 2018–19 to augment social sector spending.
- In practice, cess collections have been absorbed into general revenues.
- In FY 2023–24, only about one-fourth of the ₹71,180 crore collected through HEC went to health.
- Excluding cess contributions, Union health spending declined by 22.5% in real terms between 2020–21 and 2023–24.
Q7. What is the significance of cuts in Centrally Sponsored Health Schemes?
- The share of Union health spending transferred to States via Centrally Sponsored Schemes (CSS) declined sharply:
- From 9% (2014–15) to about 43% (2024–25).
- Flagship schemes like the National Health Mission have seen stagnation or real-term decline.
- During the NDA’s second tenure, NHM funding fell by 5% annually in real terms, weakening:
- Primary healthcare
- Rural and urban health infrastructure
- Preventive and promotive care systems
Q8. What are the implications for public health outcomes?
- Rising out-of-pocket expenditure, pushing households into poverty.
- Fiscal stress on poorer States, widening inter-State health inequalities.
- Weakening of primary and preventive healthcare, increasing long-term disease burden.
- Reduced preparedness for future health emergencies.
- These trends undermine progress towards Universal Health Coverage and health-related Sustainable Development Goals.
Q9. What are the key challenges in India’s health financing model?
- Persistent under-prioritisation of health at the Union level.
- Over-reliance on States without commensurate fiscal support.
- Ineffective earmarking and utilisation of health-related cesses.
- Declining real transfers through Centrally Sponsored Schemes.
- Mismatch between policy commitments and budgetary follow-through.
Q10. What should be the way forward to strengthen health financing?
- Re-anchor health as a national priority, not a residual budget item.
- Increase Union health expenditure in line with NHP 2017 targets.
- Ensure transparent and dedicated use of cess revenues for health.
- Revitalise NHM and CSS funding to strengthen primary healthcare.
- Enhance fiscal transfers and predictability for States, especially poorer ones.
- View health spending as productive investment in human capital, not consumption.
Conclusion
India’s health outcomes depend critically on sustained public investment. Without renewed Union leadership in health financing, rising State efforts alone cannot deliver universal, equitable, and resilient healthcare systems.